In contrast, the mortality rate was lowest (4.4%) in patients with TIMI 3 flow.83ĭespite these important associations, there are a number of limitations of the TIMI classification system. Thrombolysis and clinical outcome.83 In the Global Utilization of Streptokinase and Tissue Plasminogen Activator for Occluded Coronary Arteries (GUSTO) angiographic substudy, the mortality rate for patients with TIMI 2 flow (7.4%) was similar to the mortality rate for those with TIMI 0 or 1 flow (8.9%). Modified from Sheehan FH, Braunwald E, Canner P, et al: The effect of intravenous thrombolytic therapy on left ventricular function: A report on tissue-type plasminogen activator and streptokinase from the Thrombolysis in Myocardial Infarction (TIMI) Phase I Trial. 
Alternatively, contrast material clears from a segment distal to a stenosis noticeably more slowly than from a comparable segment not preceded by a significant stenosis.Ī small amount of contrast flows through the stenosis but fails to fully opacify the artery beyond. However, contrast enters the terminal segment perceptibly more slowly than more proximal segments. Contrast material clears as rapidly from the distal segment as from an uninvolved, more proximal segment.Ĭontrast material flows through the stenosis to opacify the terminal artery segment. TIMI Flow Grade Classificationģ (complete reperfusion) 2 (partial reperfusion)ġ (penetration with minimal perfusion) 0 (no perfusion)Īnterograde flow into the terminal coronary artery segment through a stenosis is as prompt as anterograde flow into a comparable segment proximal to the stenosis. Several throm-bolytic trials have identified an important relationship between 90-minute TIMI flow grade after 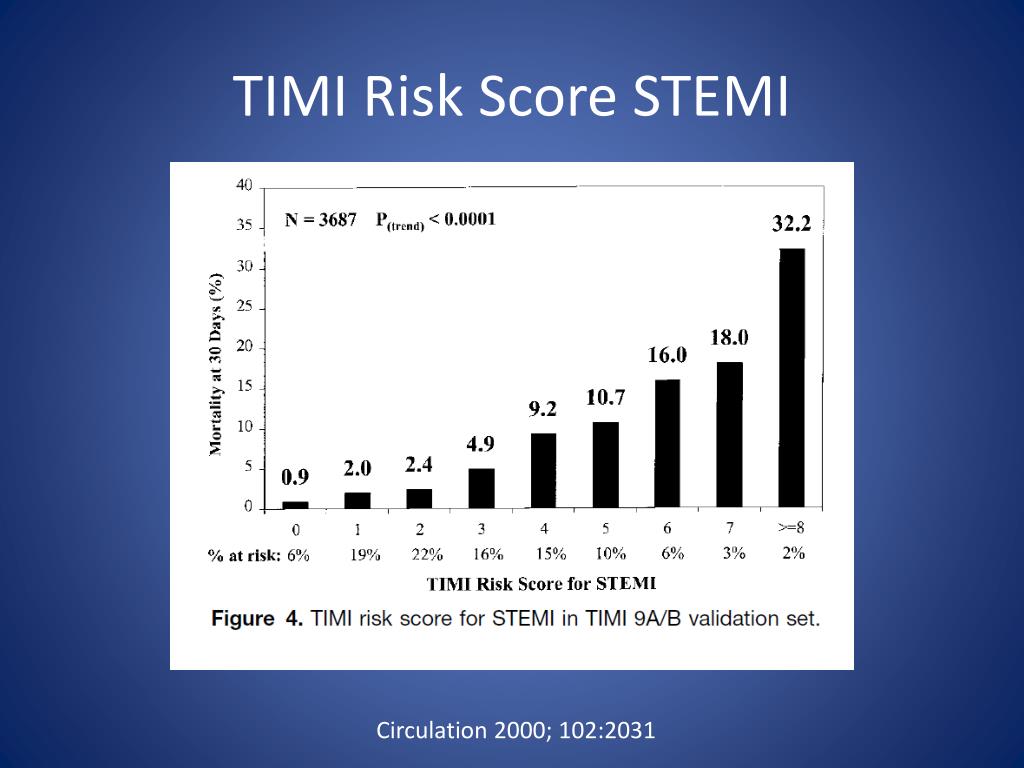
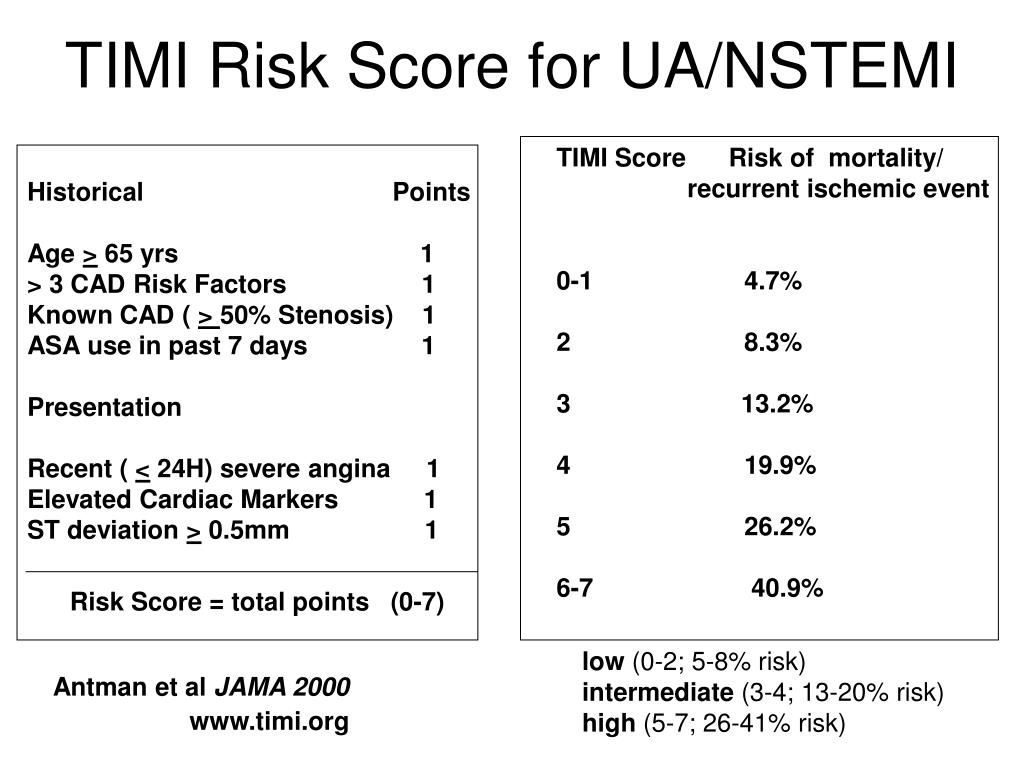
High risk patients received thrombolytic less frequently than the patients at low risk.The TIMI Flow Grade System is a valuable tool for assessing the efficacy of reperfusion strategies in patients with STEMI and for identifying patients at higher risk for an adverse outcome with acute coronary syndromes or undergoing PCI. There was a progressive increase in mortality and incidence of in-hospital complications according to the stratification by the TIMI score. The chance of receiving fibrinolytic was 50% lower in the high-risk group in relation to the low risk group (95% CI = 0.27 to 0.85, p = 0.004). The risk of death in cases of high risk was 14.1 times higher than in the cases of medium and low risk (95% CI = 4.4 to 44.1 and p <0.001). The mortality was 8.1% in the medium risk group and 55.6% in the high-risk group. In the low-risk group there was no death. The hospital mortality after infarction was 17.5%. The cases were analyzed in three risk groups according to the TIMI score. We evaluated, retrospectively, 103 cases of acute myocardial infarction with ST-segment elevation admitted to the Hospital Nossa Senhora da Conceição - Tubarão, in 20. To evaluate the management and clinical evolution of hospital inpatients with acute myocardial infarction, according to risk stratification by the TIMI score. As the risk profiles of these cases differ from those found in non-selected populations, it is important to review the applicability of the score in usual clinical conditions. The TIMI (Thrombolysis in Myocardial Infarction) risk score is derived from clinical trial involving patients who are eligible for fibrinolysis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
